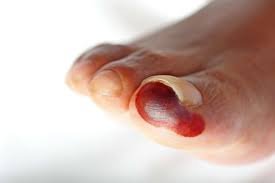
Wet gangrene is far more dangerous than dry gangrene because it involves an infection in addition to tissue death. This type typically occurs in areas where the skin has been compromised due to injury, burns, or ulcers, allowing bacteria to invade the dead tissue. The presence of bacteria causes the tissue to become swollen, moist, and often accompanied by a foul odor. Unlike dry gangrene, wet gangrene progresses rapidly and can lead to systemic infections such as sepsis, which is life-threatening if not treated promptly.
This severe infection causes the affected area to become red or dark, blistered, and excessively painful. People with compromised immune systems, diabetes, or severe injuries are at higher risk of developing wet gangrene. The bacteria release toxins which accelerate tissue destruction and provoke a strong inflammatory response, increasing swelling and fluid accumulation. Immediate medical attention is required to control the infection using intravenous antibiotics and surgical removal of necrotic tissue to prevent the spread of gangrene.
If left untreated, wet gangrene can cause septic shock and multiple organ failure. Treatment often involves supportive care to maintain blood pressure, wound care, and sometimes amputation to remove dead tissue. Preventive measures include proper wound care, early treatment of infections, and controlling underlying health conditions. Prompt medical intervention is critical to prevent severe complications and improve outcomes in cases of wet gangrene.